Mitral valve prolapse
![]() March, 27th, 2024
March, 27th, 2024
Benefit Summary
This heart condition, also called Barlow syndrome, affects the valve separating the left heart chambers. Know the symptoms and when it’s treated.
Overview
, Overview, ,
Mitral valve prolapse is a type of heart valve disease that affects the valve between the left heart chambers. The flaps (leaflets) of the mitral valve are floppy. They bulge backward (prolapse) like a parachute into the heart’s left upper chamber as the heart squeezes (contracts).
Mitral (MY-trul) valve prolapse sometimes causes blood to leak backward across the valve, a condition called mitral valve regurgitation.
Usually, mitral valve prolapse isn’t life-threatening and doesn’t require treatment or lifestyle changes. But some people may need medications or surgery, especially if the prolapse causes severe regurgitation.
Other names to describe mitral valve prolapse include:
- Barlow syndrome
- Billowing mitral valve syndrome
- Click-murmur syndrome
- Floppy valve syndrome
- Mitral prolapse
- Myxomatous mitral valve disease
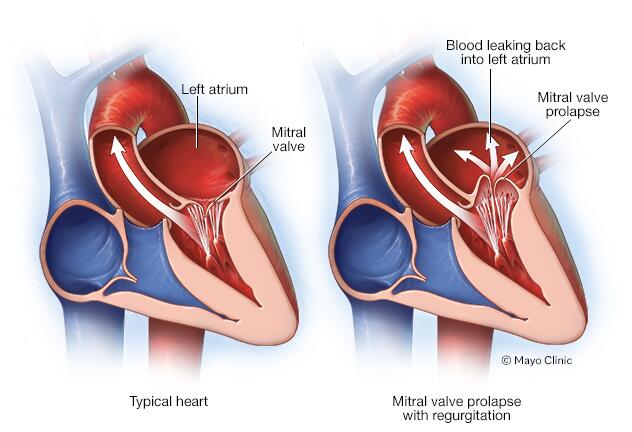
Signs and symptoms of mitral valve prolapse are due to the amount of blood leaking backward through the valve.
Mitral valve prolapse symptoms can vary widely from one person to another. Many people with mitral valve prolapse don’t have noticeable symptoms. Other people may have mild symptoms that develop gradually.
Symptoms of mitral valve prolapse may include:
- A racing or irregular heartbeat (arrhythmia)
- Dizziness or lightheadedness
- Difficulty breathing or shortness of breath, especially during exercise or when lying flat
- Fatigue
When to see a doctor
If you have symptoms of mitral valve prolapse, make an appointment with your health care provider. Many other conditions can cause similar symptoms.
If you’re having sudden or unusual chest pain or think you’re having a heart attack, seek emergency medical care immediately.
If you’ve been diagnosed with mitral valve prolapse, see your provider if your symptoms worsen.
Causes
To understand the causes of mitral valve disease, it may be helpful to know how the heart works.
The mitral valve is one of four valves in the heart that keep blood flowing in the right direction. Each valve has flaps (leaflets) that open and close once during each heartbeat. If a valve doesn’t open or close properly, blood flow through the heart to the body can be reduced.
In mitral valve prolapse, one or both of the mitral valve leaflets have extra tissue or stretch more than usual. The leaflets can bulge backward (prolapse) like a parachute into the left upper heart chamber (left atrium) each time the heart contracts to pump blood.
The bulging may keep the valve from closing tightly. If blood leaks backward through the valve, the condition is called mitral valve regurgitation.
Risk factors
Mitral valve prolapse can develop in any person at any age. Serious symptoms of mitral valve prolapse tend to occur most often in men older than 50.
Mitral valve prolapse can occur in families (be inherited) and may be linked to several other conditions, including:
- Ebstein anomaly
- Ehlers-Danlos syndrome
- Graves’ disease
- Marfan syndrome
- Muscular dystrophy
- Scoliosis
Complications
Potential complications of mitral valve prolapse may include:
- Mitral valve regurgitation. The mitral valve flaps don’t close tightly. Blood flows backward when the valve is closed, making it harder for the heart to work properly. Being male or having high blood pressure increases the risk of mitral valve regurgitation.
- Heart rhythm problems (arrhythmias). Irregular heartbeats may occur if mitral valve prolapse leads to severe regurgitation and swelling of the upper left heart chamber (atrium).
Diagnosis
To diagnose mitral valve prolapse, your health care provider will usually do a physical exam and listen to your heart with a stethoscope.
If you have mitral valve prolapse, a clicking sound may be heard through the stethoscope. If blood is leaking backward through the mitral valve, a whooshing sound (heart murmur) also may be heard.
Tests
Tests that may done to help confirm mitral valve prolapse and evaluate the heart include:
-
Echocardiogram. An echocardiogram uses sounds waves to create images of the heart in motion. A standard echocardiogram, also called a transthoracic echocardiogram (TTE), can confirm a diagnosis of mitral valve prolapse and determine its severity.
Sometimes, a transesophageal echocardiogram (TEE) may be done to get more-detailed images of the mitral valve. In this type of echocardiogram, a small transducer attached to the end of a tube is inserted down the tube leading from the mouth to the stomach (esophagus).
- Chest X-ray. A chest X-ray shows the condition of the heart and lungs. It can help show if the heart is enlarged.
- Electrocardiogram (ECG or EKG). This quick and painless test measures the electrical activity of the heart. An ECG can detect irregular heart rhythms (arrhythmias) related to mitral valve disease.
- Exercise or stress tests. These tests often involve walking on a treadmill or riding a stationary bike while the heart is monitored with ECG. Exercise tests help reveal how the heart responds to physical activity and whether mitral valve prolapse symptoms occur during exercise. If you’re unable to exercise, you might be given medications that mimic the effect of exercise on the heart.
- Cardiac catheterization. This test isn’t often used to diagnose mitral valve prolapse, but it can be helpful if other tests haven’t diagnosed the condition. A health care provider threads a thin tube (catheter) through a blood vessel in the arm or groin to an artery in the heart and injects dye through the catheter. This makes the arteries in the heart chambers show up more clearly on an X-ray.
Treatment
Most people with mitral valve prolapse, particularly people without symptoms, don’t require treatment.
If you have mitral valve regurgitation but don’t have symptoms, your health care provider may recommend regular checkups to monitor your condition.
If you have severe mitral valve regurgitation, medications or surgery may be needed even if you don’t have symptoms.
Medications
Medications may be needed to treat irregular heartbeats or other complications of mitral valve prolapse. Medications include:
- Beta blockers. These drugs relax blood vessels and slow the heartbeat, which reduces blood pressure.
- Water pills (diuretics). These medicines help remove salt (sodium) and water through your urine, reducing blood pressure.
- Heart rhythm drugs (antiarrhythmics). Medications may be used to help control irregular heart rhythms.
- Blood thinners (anticoagulants). If mitral valve disease is causing an irregular heartbeat called atrial fibrillation, your health care provider may recommend blood-thinning drugs to prevent blood clots. Atrial fibrillation increases the risk of blood clots and strokes. If you had mitral valve replacement with a mechanical valve, blood thinners are needed for life.
- Antibiotics. The American Heart Association says antibiotics aren’t usually necessary for someone with mitral valve prolapse. But if you’ve had mitral valve replacement, your care provider may recommend taking antibiotics before dental procedures to prevent a heart infection called infective endocarditis.
Surgery and other procedures
Most people with mitral valve prolapse don’t need surgery. But surgery may be recommended if mitral prolapse causes severe mitral valve regurgitation, whether or not you have symptoms.
Surgery for a diseased or damaged mitral valve includes mitral valve repair or mitral valve replacement. Mitral valve repair is preferred because it saves the existing valve.
Valve repair and replacement may be done using open-heart surgery or minimally invasive surgery. Minimally invasive surgery involves smaller incisions and may have less blood loss and a quicker recovery time.
During mitral valve repair surgery, the surgeon might remove excess tissue from the prolapsed valve so the flaps can close tightly. The surgeon may also replace the cords that support the valve. Other repairs may also be done.
If mitral valve repair isn’t possible, the valve may be replaced. During mitral valve replacement surgery, a surgeon removes the mitral valve and replaces it with a mechanical valve or a valve made from cow, pig or human heart tissue (biological tissue valve).
Sometimes, a heart catheter procedure is done to place a replacement valve into a biological tissue valve that no longer works well. This is called a valve-in-valve procedure.
Self care
If you have mitral valve prolapse, you’ll have regular follow-up appointments with your health care provider to monitor your condition.
It’s also important to take steps to keep your heart healthy.
- Eat a heart-healthy diet. Eat a variety of fruits and vegetables. Choose low-fat or fat-free dairy products, poultry, fish, and whole grains. Avoid saturated and trans fat, and excess salt and sugar.
- Maintain a healthy weight. If you are overweight or have obesity, your health care provider might recommend that you lose weight.
- Get regular physical activity. Most people with mitral valve prolapse are able to do daily activities and exercise without restrictions. Aim to include about 30 minutes of physical activity, such as brisk walks, into your daily fitness routine. If mitral valve prolapse causes severe regurgitation, your provider may recommend certain exercise limitations.
- Manage stress. Getting more exercise, connecting with others and practicing mindfulness are some ways to reduce stress.
- Avoid tobacco. If you smoke, quit. Ask your health care provider about resources to help you quit smoking.
Preparing for your appointment
Here’s some information to help you get ready for your appointment.
What you can do
- Be aware of any pre-appointment restrictions. At the time you make the appointment, be sure to ask if there’s anything you need to do in advance.
- Write down your symptoms, including any that may seem unrelated to mitral valve prolapse, and when they began.
- Write down key personal information, including a family history of heart disease, heart defects, genetic disorders, strokes, high blood pressure or diabetes, and any major stresses or recent life changes.
- Make a list of all medications, vitamins or supplements you take, including doses.
- Take a family member or friend along, if possible. Someone who accompanies you can help you remember the information you’re given.
- Be prepared to discuss your diet and exercise habits. If you don’t already follow a diet or exercise routine, be ready to talk to your health care provider about any challenges you might face in getting started.
- Write down questions to ask your provider.
For mitral valve prolapse, some basic questions to ask your health care provider include:
- What is likely causing my symptoms or condition?
- What are other possible causes?
- What tests do I need?
- Do I need treatment? What kind?
- What are the alternatives to the primary approach that you’re suggesting?
- I have other health conditions. How can I best manage them together?
- Are there any restrictions that I need to follow?
- Should I see a specialist?
- If I need surgery, which surgeon do you recommend for mitral valve repair?
- Is there a generic alternative to the medicine you’re prescribing for me?
- Are there any brochures or other printed material that I can take home with me? What websites do you recommend visiting?
Don’t hesitate to ask any questions you have.
What to expect from your doctor
Your health care provider is likely to ask you questions, such as:
- Do you always have symptoms or do they come and go?
- How severe are your symptoms?
- What makes the symptoms better?
- What makes the symptoms worse?
© 1998-2025 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



