Gangrene
![]() February, 22nd, 2024
February, 22nd, 2024
Benefit Summary
A severe bacterial infection or lack of blood flow can cause body tissue to die. Know the warning signs and symptoms of this life-threatening condition.
Overview
, Overview, ,
Gangrene is death of body tissue due to a lack of blood flow or a serious bacterial infection. Gangrene commonly affects the arms and legs, including the toes and fingers. It can also occur in the muscles and in organs inside the body, such as the gallbladder.
A condition that can damage the blood vessels and affect blood flow, such as diabetes or hardened arteries (atherosclerosis), increases the risk of gangrene.
Treatments for gangrene may include antibiotics, oxygen therapy, and surgery to restore blood flow and remove dead tissue. The earlier gangrene is identified and treated, the better the chances for recovery.
Symptoms
When gangrene affects the skin, signs and symptoms may include:
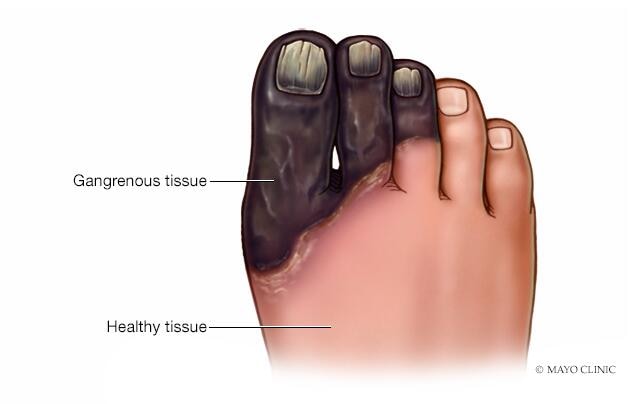
- Changes in skin color — ranging from pale gray to blue, purple, black, bronze or red
- Swelling
- Blisters
- Sudden, severe pain followed by a feeling of numbness
- A foul-smelling discharge leaking from a sore
- Thin, shiny skin, or skin without hair
- Skin that feels cool or cold to the touch
If gangrene affects tissues beneath the surface of your skin, such as gas gangrene or internal gangrene, you may also have a low-grade fever and generally feel unwell.
If the germs that caused the gangrene spread through the body, a condition called septic shock can occur. Signs and symptoms of septic shock include:
- Low blood pressure
- Fever, although some people may have a body temperature lower than 98.6 F (37 C)
- Rapid heart rate
- Lightheadedness
- Shortness of breath
- Confusion
When to see a doctor
Gangrene is a serious condition and needs emergency treatment. Call your health care provider immediately if you have persistent, unexplained pain in any area of your body along with one or more of the following signs and symptoms:
- Persistent fever
- Skin changes — including discoloration, warmth, swelling, blisters or lesions — that won’t go away
- A foul-smelling discharge leaking from a sore
- Sudden pain at the site of a recent surgery or trauma
- Skin that’s pale, hard, cold and numb
Causes
Causes of gangrene include:
- Lack of blood supply. The blood provides oxygen and nutrients to the body. It also provides the immune system with antibodies to fight infections. Without a proper blood supply, cells can’t survive, and tissue dies.
- Infection. An untreated bacterial infection can cause gangrene.
- Traumatic injury. Gunshot wounds or crushing injuries from car crashes can cause open wounds that let bacteria into the body. If the bacteria infect tissues and remain untreated, gangrene can occur.
Types of gangrene
- Dry gangrene. This type of gangrene involves dry and shriveled skin that looks brown to purplish blue or black. Dry gangrene may develop slowly. It occurs most commonly in people who have diabetes or blood vessel disease, such as atherosclerosis.
-
Wet gangrene. Gangrene is referred to as wet if bacteria have infected the tissue. Swelling, blistering and a wet appearance are common features of wet gangrene.
Wet gangrene may develop after a severe burn, frostbite or injury. It often occurs in people with diabetes who unknowingly injure a toe or foot. Wet gangrene needs to be treated immediately because it spreads quickly and can be deadly.
-
Gas gangrene. Gas gangrene typically affects deep muscle tissue. The surface of your skin may look normal at first.
As the condition worsens, the skin may become pale and then turn other colors such as gray or purplish red. The skin may look bubbly. It may make a crackling sound when you press on it because of the gas within the tissue.
Gas gangrene is most commonly caused by bacteria called Clostridium perfringens. Bacteria gather in an injury or surgical wound that has no blood supply. The bacterial infection produces toxins that release gas and cause tissue death. Like wet gangrene, gas gangrene is a life-threatening condition.
- Internal gangrene. Internal gangrene affects one or more of the organs, such as the intestines, gallbladder or appendix. It occurs when blood flow to an internal organ is blocked. For example, it may happen if the intestines bulge through a weakened area of muscle in the stomach area (hernia) and become twisted. Left untreated, internal gangrene can be deadly.
- Fournier’s gangrene. This type of gangrene involves the genital organs. It usually affects men, but women also can get it. An infection in the genital area or urinary tract causes this type of gangrene.
- Meleney’s gangrene. This is a rare type of gangrene. It’s usually a complication of surgery. Painful skin lesions typically occur one to two weeks after a surgery. Another name for this condition is progressive bacterial synergistic gangrene.
Things that can increase the risk of gangrene include:
- Diabetes. High blood sugar levels can eventually damage blood vessels. Blood vessel damage can slow or block blood flow to a part of the body.
- Blood vessel disease. Hardened and narrowed arteries (atherosclerosis) and blood clots can block blood flow to an area of the body.
- Severe injury or surgery. Any process that causes trauma to the skin and underlying tissue, including frostbite, increases the risk of gangrene. The risk is greater if you have an underlying condition that affects blood flow to the injured area.
- Smoking. People who smoke have a higher risk of gangrene.
- Obesity. Extra weight can push on arteries, slowing blood flow and increasing the risk of infection and poor wound healing.
- Immunosuppression. Chemotherapy, radiation and certain infections, such as human immunodeficiency virus (HIV), can affect the body’s ability to fight off infections.
- Injections. Rarely, injectable drugs have been linked to infection with bacteria that cause gangrene.
- Complications of COVID-19. There have been a few reports of people getting dry gangrene in their fingers and toes after having COVID-19-related blood clotting problems (coagulopathy). More research is needed to confirm this link.
Complications
Gangrene can lead to serious complications if it’s not immediately treated. Bacteria can spread quickly to other tissues and organs. You may need to have a body part removed (amputated) to save your life.
Removal of infected tissue can lead to scarring or the need for reconstructive surgery.
Prevention
Here are a few ways to help reduce the risk of developing gangrene:
- Manage diabetes. If you have diabetes, it’s important to control your blood sugar levels. Also make sure you examine your hands and feet daily for cuts, sores and signs of infection, such as redness, swelling or drainage. Ask your health care provider to check your hands and feet at least once a year.
- Lose weight. Extra pounds raise the risk of diabetes. The weight also puts pressure on the arteries, slowing blood flow. Decreased blood flow increases infection risk and causes slow wound healing.
- Don’t smoke or use tobacco. Long-term of tobacco damages the blood vessels.
- Wash your hands. Practice good hygiene. Wash any open wounds with a mild soap and water. Keep the hands clean and dry until they heal.
- Check for frostbite. Frostbite reduces blood flow in the affected body area. If you have skin that’s pale, hard, cold and numb after being in cold temperatures, call your care provider.
Diagnosis
Tests used to help diagnose gangrene include:
- Blood tests. A high white blood cell count is often a sign of infection. Other blood tests can be done to check for the presence of specific bacteria and other germs.
- Fluid or tissue culture. Tests can be done to look for bacteria in fluid sample from a skin blister. A sample of tissue can be examined under a microscope for signs of cell death.
- Imaging tests. X-rays, computerized tomography (CT) scans and magnetic resonance imaging (MRI) scans can show the organs, blood vessels and bones. These tests can help show how far gangrene has spread through the body.
- Surgery. Surgery may be done to get a better look inside the body and learn how much tissue is infected.
Treatment
Tissue that has been damaged by gangrene can’t be saved. But treatment is available to help prevent gangrene from getting worse. The faster you get treatment, the better your chance for recovery.
Treatment for gangrene may include one or more of the following:
- Medication
- Surgery
- Hyperbaric oxygen therapy
Medications
Medications to treat a bacterial infection (antibiotics) are given by IV or taken by mouth.
Pain medications may be given to relieve discomfort.
Surgery or other procedures
Depending on the type of gangrene and its severity, more than one surgery may be needed. Surgery for gangrene includes:
- Debridement. This type of surgery is done to remove the infected tissue and stop the infection from spreading.
- Vascular surgery. Surgery may be done to repair any damaged or diseased blood vessels to restore blood flow to the infected area.
- Amputation. In severe cases of gangrene, the infected body part — such as a toe, finger, arm or leg — may need to be surgically removed (amputated). You may later be fitted with an artificial limb (prosthesis).
- Skin grafting (reconstructive surgery). Sometimes, surgery is needed to repair damaged skin or to improve the appearance of gangrene-related scars. Such surgery may be done using a skin graft. During a skin graft, the surgeon removes healthy skin from another part of the body and places it over the affected area. A skin graft can be done only if there is enough blood supply to the area.
Hyperbaric oxygen therapy
Hyperbaric oxygen therapy is done inside a chamber pressurized with pure oxygen. You usually lie on a padded table that slides into a clear plastic tube. The pressure inside the chamber will slowly rise to about 2.5 times regular atmospheric pressure.
Hyperbaric oxygen therapy helps the blood carry more oxygen. Oxygen-rich blood slows the growth of bacteria that live in tissue lacking oxygen. It also helps infected wounds heal more easily.
A hyperbaric oxygen therapy session for gangrene usually lasts about 90 minutes. Two to three treatments a day may be needed until the infection clears.
Preparing for your appointment
Call your health care provider right away if you have symptoms of gangrene. Depending on the severity of your symptoms, you may be told to go to the emergency room or to call 911 or your local emergency number for medical help.
If you have time before you leave home or on the way to the hospital, use the information below to prepare for your visit.
What you can do
- Write down any symptoms you have and how long you’ve had them Note as many details as possible about when your symptoms first appeared. Include how they may have worsened or spread over time.
- Write down any recent injury or trauma to your skin, including cuts, bites, injections, surgery or possible frostbite. If you’ve recently used injectable drugs, tell the health care provider.
- Write down important medical information, including any other conditions you have.
- List any medications, vitamins or supplements that you’re taking. Include their doses.
- Take a family member or friend along. Gangrene is a medical emergency. Take someone with you to help you remember all the information you receive. You’ll also want someone who can stay with you if you need immediate treatment.
- Write down questions to ask your health care provider.
For gangrene, some basic questions to ask your health care provider include:
- What’s the most likely cause of my symptoms or condition?
- What kinds of tests do I need?
- Do I need to stay in the hospital?
- What treatments do I need?
- How soon will treatment work?
- Will I have a full recovery? If so, how long will recovery take?
- Am I at risk of long-term complications?
Don’t hesitate to ask your care provider any additional questions.
What to expect from your doctor
Your health care provider is likely to ask several questions to help determine the diagnosis and treatment. You may be asked:
- What are your symptoms?
- When did the symptoms start?
- How painful is the affected area?
- Do the symptoms seem to be spreading or getting worse?
- Have you had any recent injuries or trauma to your skin, such as cuts, wounds, bites or surgery?
- Have you been in very cold temperatures that made your skin change color or turn numb?
- Do you use injectable drugs, including illegal drugs?
- Have you been diagnosed with any other medical conditions?
- What medications are you taking or have recently taken, including prescription drugs, over-the-counter medications, herbs and supplements?
© 1998-2025 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



