Breast MRI
![]() November, 20th, 2024
November, 20th, 2024
Summary
Learn more about how this imaging test helps diagnose cancer and when it’s used.
Overview
, Overview, ,
Magnetic resonance imaging (MRI) of the breast, also called breast MRI, is a test used to find breast cancer. It also can help rule out breast cancer when there are other problems in the breast.
A breast MRI makes pictures of the inside of the breast. It uses powerful magnets, radio waves and a computer to make images with a lot of detail.
A breast MRI might be done after a biopsy shows cancer. Breast MRI can show the extent of the cancer or an issue with the other breast.
Breast MRI also may be used with mammography as a screening tool for detecting breast cancer in some people. This includes people with a high risk of breast cancer. It also includes people who have a strong family history of breast cancer or who have breast cancer gene changes that were passed down through the family, called inherited.
Why it’s done
A breast MRI is used to see if there are other areas within the breast that also could have cancer. It’s also used to screen for breast cancer in people who have a high risk of getting breast cancer in their lifetimes.
Your health care provider may recommend a breast MRI if there is:
- More cancer in the breast or cancer in the other breast after a breast cancer diagnosis.
- A possible leak or tear of a breast implant.
- A high risk of breast cancer. This means lifetime risk of 20% or more. Risk tools that look at family history and other risk factors work out lifetime risk.
- A strong family history of breast cancer or ovarian cancer.
- Very dense breast tissue, and mammograms missed an earlier breast cancer.
- A history of breast changes that could lead to cancer, a strong family history of breast cancer and dense breast tissue. Breast changes might include a buildup of unusual cells in the breast, called atypical hyperplasia, or unusual cells in the milk glands of the breast, call lobular carcinoma in situ.
- A breast cancer gene change passed through families, called inherited. Gene changes can include BRCA1 or BRCA2, among others.
- A history of radiation treatments to the chest area between the ages of 10 and 30 years.
If you don’t know if you might be at high risk, ask a member of your care team to help you find out what your risk is. You might be sent to a breast clinic or breast-health specialist. A specialist can talk to you about your risk and your screening choices, as well as ways to lower your risk for getting breast cancer.
A breast MRI is meant to be used with a mammogram or other breast-imaging test. It’s not to be used instead of a mammogram. Although it’s a good test, a breast MRI can still miss some breast cancers that a mammogram will find.
A breast MRI may be ordered once a year in high-risk women around the same time as the screening mammogram. Very high-risk women may be screened by having either a breast MRI or mammogram every 6 months.
Risks
A breast MRI is safe. It doesn’t use radiation. But as with other tests, a breast MRI has risks, such as:
- False-positive results. A breast MRI might show a need for more testing. More testing, such as a breast ultrasound or breast biopsy, might show no cancer. These results are called false-positives. A false-positive result may lead to worry and tests that aren’t needed.
- Reaction to the contrast dye used. A breast MRI involves a dye called gadolinium that’s given through a vein to make the images easier to see. This dye can cause allergic reactions. And it can cause serious complications for people with kidney problems.
How you prepare
To prepare for a breast MRI, you need to take these steps:
-
Schedule the MRI for the beginning of your menstrual cycle. If you haven’t yet reached menopause, the MRI facility may prefer to schedule your MRI at a certain time during your menstrual cycle, around days 5 to 15.
The first day of your period is day one of your cycle. Let the facility know where you are in your cycle so that your breast MRI appointment can be made at the best time for you.
- Tell a member of your health care team about your allergies. Most MRI procedures use a dye called gadolinium to make the images easier to see. The dye is given through a vein in the arm. Letting a member of your team know about your allergies can help prevent problems with the dye.
- Tell a member of your health care team if you have kidney problems. A dye often used for MRI images called gadolinium can cause serious problems in people with kidney issues.
- Tell a member of your health care team if you’re pregnant. An MRI generally isn’t recommended for people who are pregnant. This is because of possible risk of the dye to the baby.
-
Tell a member of your health care team if you’re nursing. If you’re nursing, you might want to stop nursing for two days after you have the MRI. The American College of Radiology states that the risk to babies from the contrast dye is low. But, if you’re worried, stop breastfeeding for 12 to 24 hours after the MRI.
This will give your body time to get rid of the dye. You can pump and discard your milk during this time. Before the MRI, you can pump and store milk to feed your baby.
- Don’t wear anything with metal during the MRI. An MRI can damage metal, such as in jewelry, hairpins, watches and eyeglasses. Leave things made of metal at home or take them off before your MRI
- Tell a member of your health care team about medical devices that have been put into your body, called implanted. Implanted medical device include pacemakers, defibrillators, implanted drug ports or artificial joints.
What you can expect
When you get to your appointment, you might get a gown or robe to wear. You’ll take off your clothes and jewelry. If you have trouble being in a small space, tell a member of your health care team before your breast MRI. You may be given medicine to relax you.
A dye, also called a contrast agent, might be put through a line in your arm, called intravenous (IV). The dye makes the tissues or blood vessels on the MRI pictures easier to see.
The MRI machine has a large, central opening. During the breast MRI, you lie face down on a padded table. Your breasts fit into a hollow space in the table. The space has coils that get signals from the MRI machine. The table then slides into the opening of the machine.
The MRI machine makes a magnetic field around you that sends radio waves to your body. You won’t feel anything. But you may hear loud tapping and thumping sounds from inside the machine. Because of the loud noise, you may get earplugs to wear.
The person doing the test watches you from another room. You can speak to the person through a microphone. During the test, breathe normally and lie as still as you can.
The breast MRI appointment may take 30 minutes to one hour.
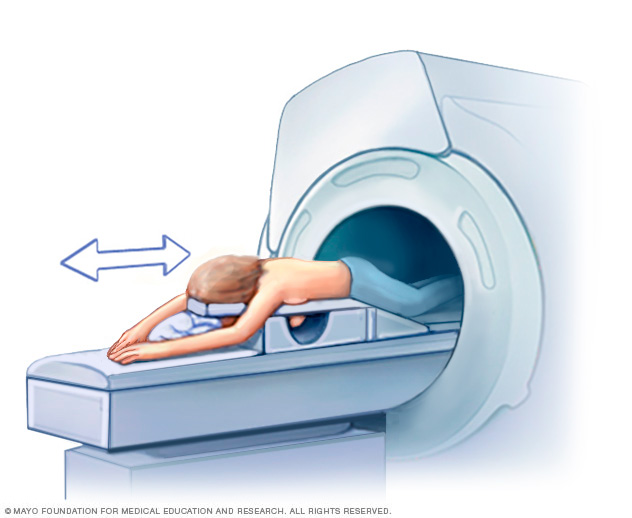
Getting a breast MRI involves lying face down on a padded scanning table. The breasts fit into a hollow space in the table. The hollow has coils that get signals from the MRI. The table slides into the large opening of the MRI machine.
Breast MRI Results
A doctor specializing in imaging tests, called a radiologist, reviews the pictures from the breast MRI. A member of your health care team talks to you about the results of the test.

A breast MRI can find problem areas within the breast. A breast biopsy might follow a breast MRI to see if the problem areas found on the MRI are cancer.

A breast MRI can find problem areas within the breast. A breast biopsy might follow a breast MRI to see if the problem areas found on the MRI are cancer.
, Breast MRI results,
© 1998-2025 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved. Terms of Use



